This article provides an overview of the medically important Clostridium species and their impact on human health. It explains how these anaerobic, spore-forming bacteria produce potent toxins that lead to serious diseases. The major infections include tetanus, gas gangrene, botulism, food poisoning, and antibiotic-associated colitis.
The genus Clostridium
Clostridium is a genus of Gram-positive, rod-shaped, spore-forming bacteria that grow in anaerobic (oxygen-free) environments. These microorganisms are commonly present in soil, water, dust, and the digestive tracts of humans and animals. An important feature that makes them highly resilient is their ability to form endospores, enabling survival under extreme conditions such as heat, dryness, and chemical exposure.
While many species are harmless, several are clinically important because they release potent toxins capable of causing serious human illnesses. Clostridial infections typically occur when spores enter the body through wounds, contaminated food, or disturbances in the normal gut microbiota. Diseases such as tetanus, botulism, gas gangrene, and antibiotic-associated colitis highlight the medical significance of this group of bacteria.
Clostridium tetani and Tetanus
Clostridium tetani is the bacterium responsible for tetanus. A distinctive feature of this organism is the formation of a terminal endospore (Figure 1) that gives the cell a characteristic drumstick-like shape. Its primary virulence factor is a potent neurotoxin. The bacterium commonly inhabits soil and the intestinal tracts of grazing animals. When its spores enter wounds that provide favorable anaerobic conditions, especially deep, contaminated injuries with damaged tissue and the presence of other bacteria, it can grow and release its toxin.
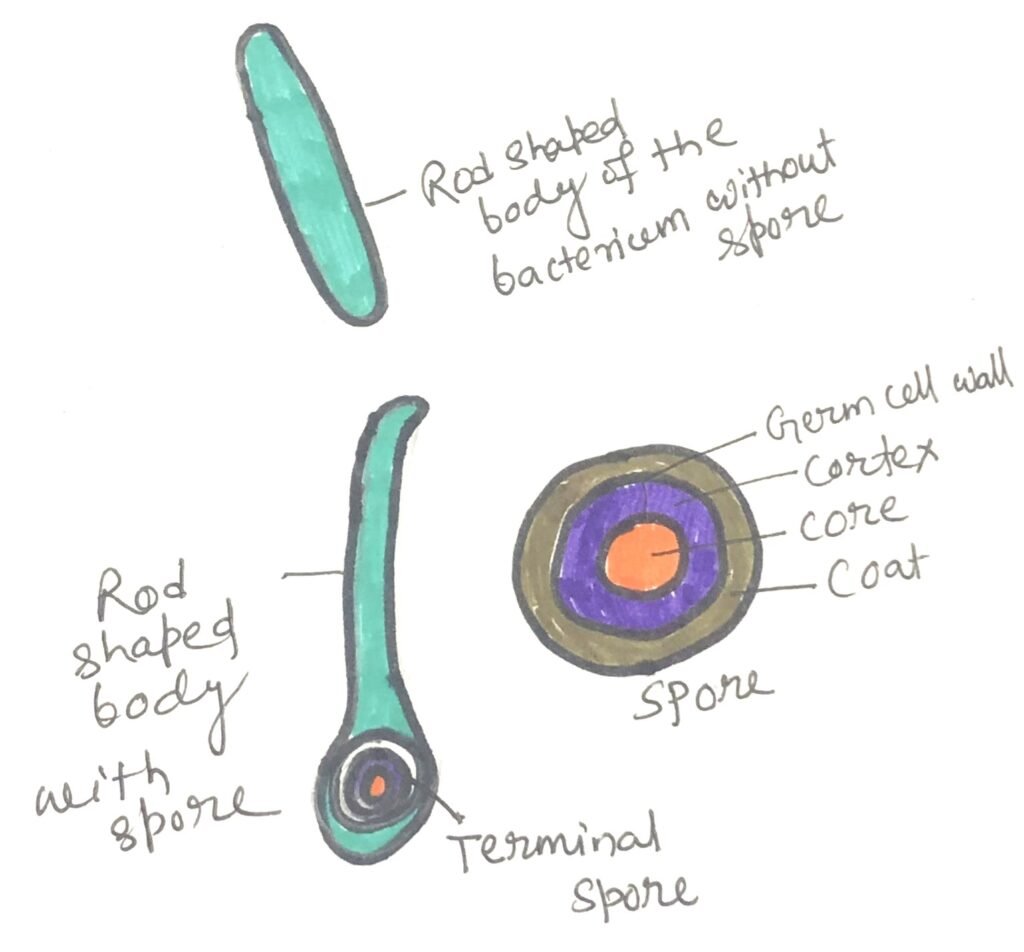
Once produced, the toxin attaches to nearby motor nerve endings and travels to the central nervous system. This leads to severe muscle stiffness and painful spasms, particularly affecting the jaw and neck. As the disease progresses, paralysis of the chest muscles may occur, often resulting in respiratory or cardiac failure. The fatality rate ranges from about 55–65%.
Treatment includes the administration of muscle relaxants and antitoxin to neutralize any circulating toxin that has not yet bound to nerve tissue. Prevention relies on vaccination with tetanus toxoid, which stimulates the formation of protective antibodies. Booster doses are recommended every ten years to maintain immunity. In individuals who are not vaccinated and sustain high-risk wounds, immediate administration of tetanus antitoxin is essential to prevent disease development.
Clostridium perifringens: Gas Gangrene and Food Poisoning
Several species of Clostridium are capable of causing gas gangrene in humans. However, most infections are attributed to Clostridium perfringens type A, a bacterium that normally exists in the human intestinal flora. Its disease-causing ability is largely due to multiple toxins, including α, θ, κ, µ, and γ toxins. The α toxin acts as a phospholipase that disrupts the cell membranes of red blood cells and tissues. The θ toxin functions as an oxygen-sensitive hemolysin, while the κ toxin breaks down connective tissue through collagen degradation. The µ toxin (a hyaluronidase) enhances the spread of infection, and the γ toxin acts as a deoxyribonuclease.
Gas gangrene typically develops when wounds become contaminated with the organism, similar to tetanus infections. The disease is marked by severe toxemia accompanied by gas production within infected tissues. Because the bacterium spreads rapidly and aggressively, prevention is critical and includes prompt surgical removal of dead tissue and clots, administration of antitoxin, and use of antibiotics to control bacterial growth. Once the infection becomes established, the rapid spread may necessitate amputation of the affected limb to save the patient’s life. Hyperbaric oxygen therapy is another treatment option, in which patients are exposed to high-pressure oxygen to increase tissue oxygen levels and inhibit bacterial growth. However, if toxins have already spread widely in the body, treatment may not be successful.
In addition to wound infections, C. perfringens is a common cause of food poisoning. Spores may survive in improperly cooked meat or poultry, especially when food is held at warm temperatures for extended periods. After consumption, the bacteria multiply in the intestine and produce an enterotoxin during sporulation. This toxin leads to abdominal cramps, diarrhea, and occasionally nausea and vomiting. Symptoms usually appear 8–24 hours after eating contaminated food and typically resolve within 12–18 hours.
Clostridium botulinum and Botulism
Clostridium botulinum (figure 2) is responsible for botulism, a serious paralytic illness that affects both humans and animals. The disease usually occurs after consuming food contaminated with a powerful neurotoxin produced by the bacterium. This species is classified into seven serological types (A–G), each producing a distinct toxin. Human botulism is most commonly linked to types A, B, and E, and rarely type F. Spores of types A and B are frequently present in soil, while type E is mainly found in aquatic sediments, particularly in regions such as the Great Lakes, the western coasts of North America, and northern Japan, where fish and seafood products may become contaminated.
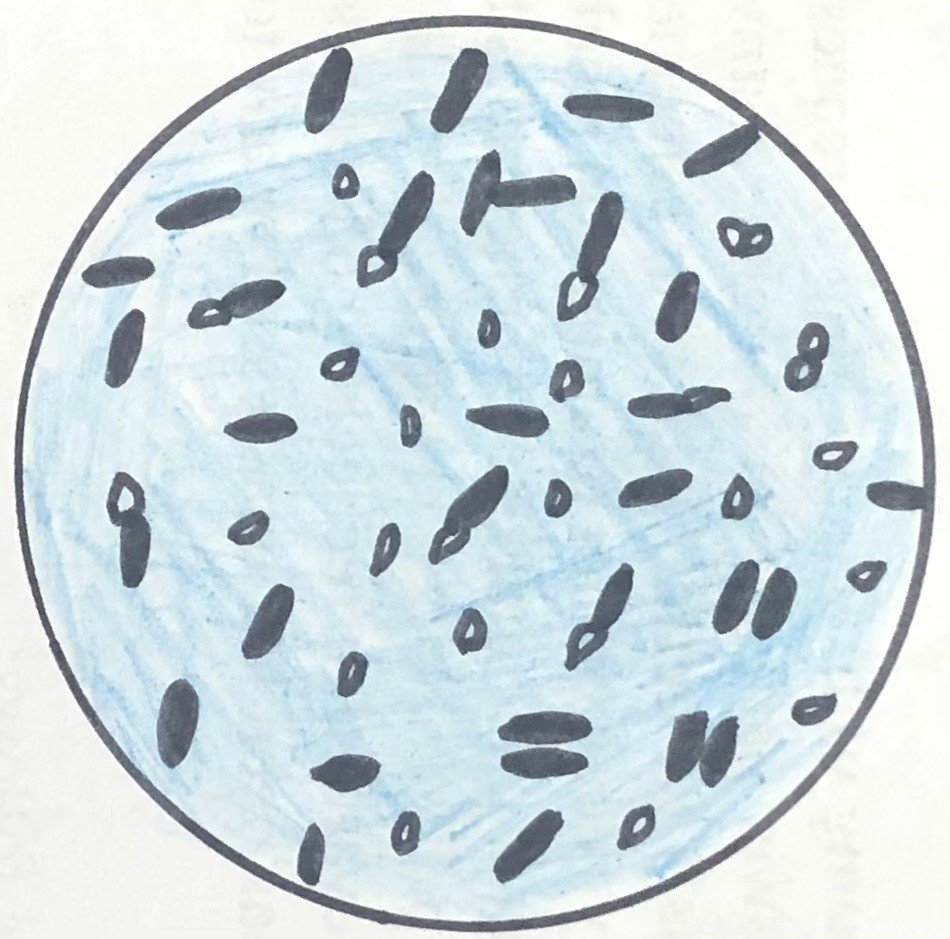
Treatment involves administration of a polyvalent antitoxin to neutralize any circulating toxin that has not yet attached to nerve tissue. In severe cases, patients with breathing difficulties may require mechanical ventilation to prevent respiratory failure.
A separate form known as infant botulism occurs in babies between two weeks and six months of age. Since the normal intestinal microbiota in infants is not fully developed, ingested spores can germinate and produce toxins within the intestine. This results in symptoms such as lethargy, excessive sleepiness, weak muscle tone, poor head control, and slowed reflexes. In difficult situations, breathing problems and death may occur if treatment is not provided.
Clostridium difficile and Pseudomembranous Colitis
In healthy adults, Clostridium difficile is usually absent or present only in very small numbers in the intestine. However, treatment with broad-spectrum antibiotics such as ampicillin, clindamycin, chloramphenicol, tetracyclines, and cephalosporins can disrupt the normal gut microbiota. This imbalance allows the bacterium to multiply rapidly and cause a serious colon infection known as pseudomembranous colitis.
The illness is marked by watery diarrhea, inflammation of the colon, and the formation of a characteristic pseudomembrane on the intestinal lining. If left untreated, the mortality rate can range from approximately 27% to 44%. Oral administration of vancomycin is generally effective in managing the infection.
The disease is mainly driven by two exotoxins. Toxin A acts as an enterotoxin that promotes fluid accumulation in the intestine, while toxin B functions as a cytotoxin that damages and destroys the cells of the intestinal wall.
Conclusion
Members of the genus Clostridium represent some of the most important toxin-producing bacterial pathogens affecting humans. Although many species exist harmlessly in the environment or as part of normal microbiota, certain members can cause severe and life-threatening illnesses when favorable conditions allow them to grow and release potent toxins. Diseases such as tetanus, gas gangrene, botulism, food poisoning, and antibiotic-associated colitis demonstrate the wide range of health problems linked to these anaerobic bacteria.
A common theme among these infections is the role of spores, toxin production, and conditions that disrupt normal body defenses, such as wounds, contaminated food, or antibiotic use. Fortunately, many clostridial diseases can be prevented or managed through vaccination, proper wound care, safe food handling, responsible antibiotic use, and timely medical treatment. Continued awareness and research remain essential to reduce the impact of these powerful bacterial pathogens on human health.
You may also like:
- Bacterial Exotoxins and Their Pathogenic Effects
- Endotoxins and Associated Virulence Determinants in Bacterial Pathogenesis
- Aerobic Gram Negative Rods as Human Pathogens

I, Swagatika Sahu (author of this website), have done my master’s in Biotechnology. I have around fourteen years of experience in writing and believe that writing is a great way to share knowledge. I hope the articles on the website will help users in enhancing their intellect in Biotechnology.
