This article briefly describes aerobic gram-negative rods as human pathogens, explaining their characteristics, major genera, disease-causing mechanisms, and their importance in diagnosis, treatment, and prevention of infections. Aerobic gram-negative rods form a diverse group of bacteria capable of surviving in oxygen-rich environments and causing a wide range of human infections. Key genera such as Pseudomonas, Legionella, Brucella, and Bordetella possess unique virulence mechanisms that help them invade hosts and evade immune defenses. Understanding their characteristics is essential for accurate diagnosis, treatment, and prevention of the diseases they cause.
Pseudomonas aeruginosa in Human Infections
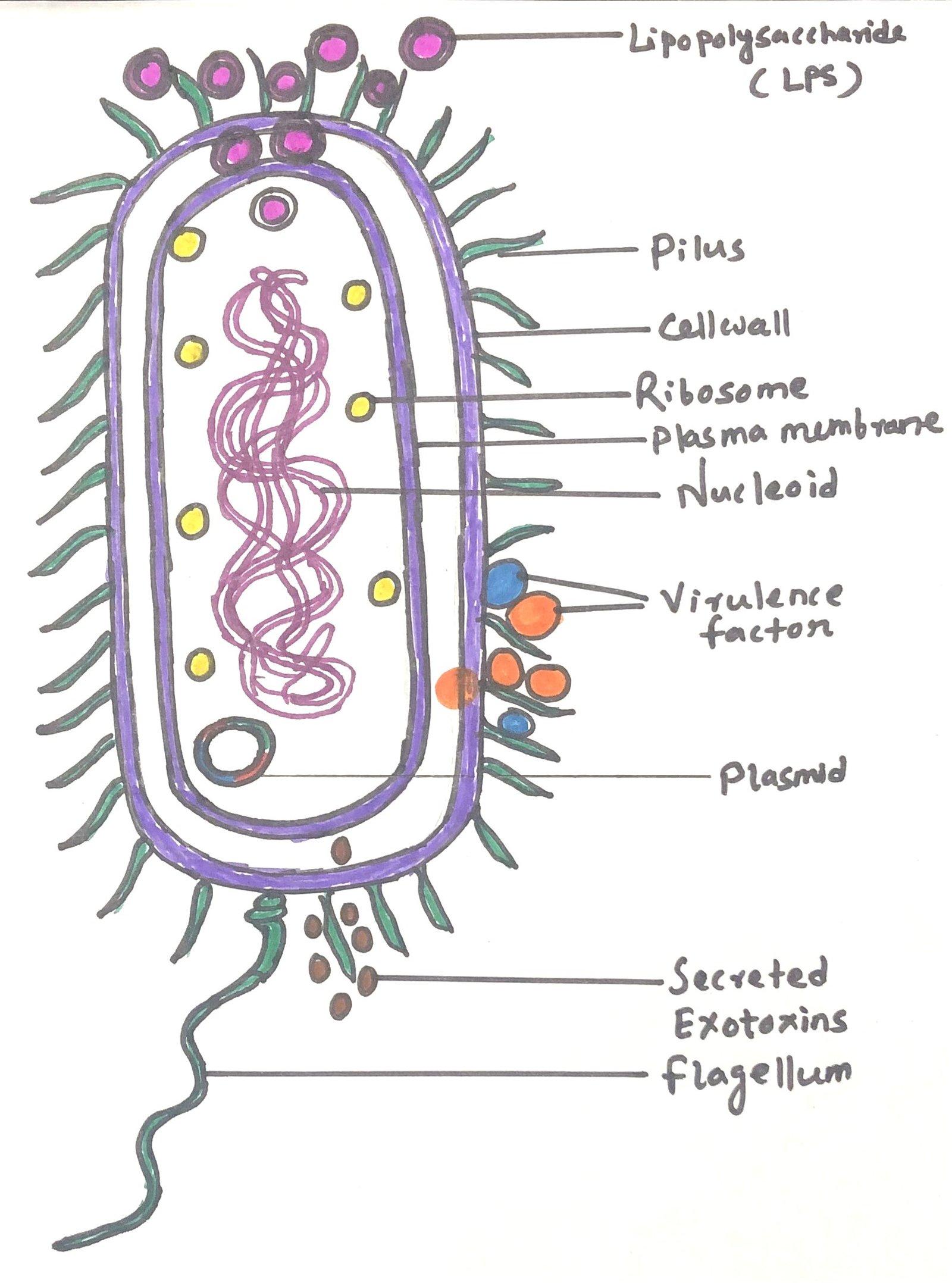
The genus Pseudomonas includes a diverse group of bacteria widely distributed in natural environments such as soil and water. Many species act as opportunistic pathogens, causing disease primarily in individuals with weakened immune defenses or in hospital settings. Among them, Pseudomonas aeruginosa (Figure 1) stands out as the most clinically significant species in human infections.
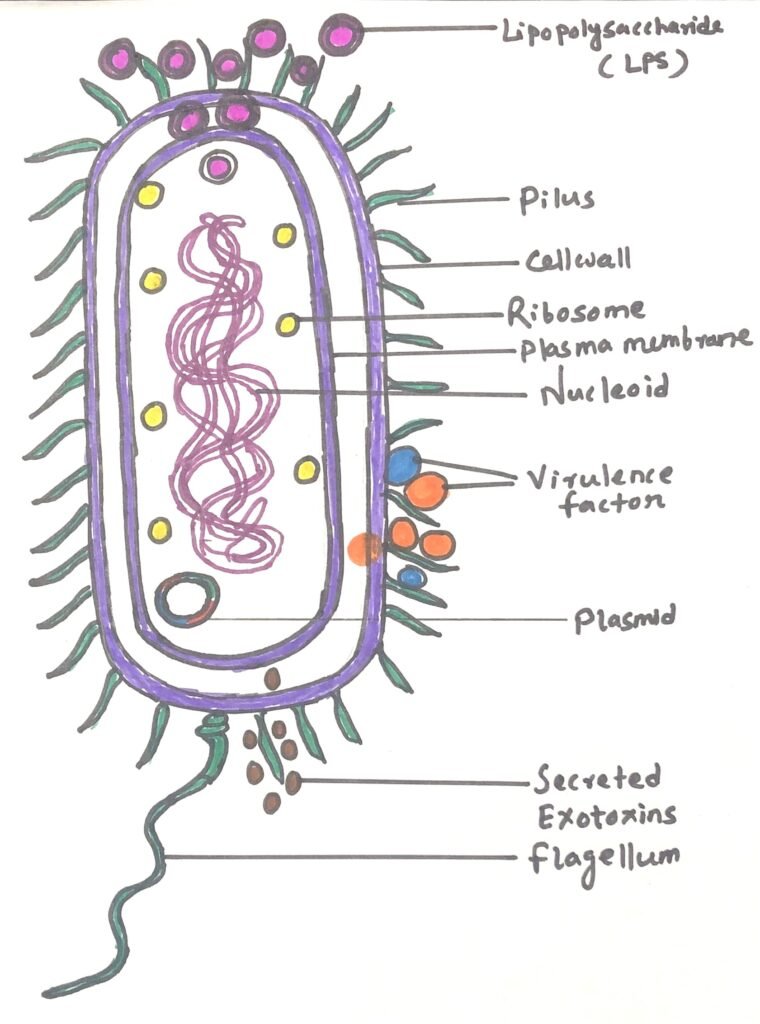
Some species within the genus primarily affect animals. Pseudomonas mallei is an obligate parasite that survives only within animal hosts and causes glanders, a disease affecting many warm-blooded animals. Pseudomonas pseudomallei, commonly found in tropical and subtropical soils, is responsible for melioidosis, which can infect both animals and humans.
In human medicine, Pseudomonas aeruginosa is the species most frequently isolated from clinical samples. It produces several virulence factors, including endotoxin, exotoxin A, tissue-damaging enzymes, and protective polysaccharides that help the bacterium evade immune responses. This organism thrives in moist environments and can persist on various hospital surfaces and equipment, making it a major cause of hospital-acquired infections. It is commonly associated with infections following surgery, burns, and urinary catheterization, and it poses a serious risk to individuals receiving immunosuppressive treatments or those with cystic fibrosis. Its natural resistance to many antibiotics further complicates treatment and contributes to its clinical importance.
Legionella and the Spectrum of Legionellosis
Legionella are small Gram-negative rods that cause legionellosis, a respiratory infection acquired mainly from environmental sources such as contaminated water systems. Person-to-person transmission is considered rare. The disease gained recognition after a major pneumonia outbreak in 1976 during an American Legion convention in Philadelphia, which led to the eventual isolation and identification of the bacterium.
Among the species, Legionella pneumophila is the most clinically important and is responsible for two distinct disease forms. The first is Legionnaires’ disease, a severe form of bronchopneumonia marked by fever, chills, dry cough, and sometimes gastrointestinal or neurological symptoms, with a relatively high mortality rate. The second is Pontiac fever, a milder, self-limiting illness characterized by flu-like symptoms.
Because Legionella species are widespread in water systems, controlling infections can be challenging. Preventive strategies often focus on maintaining and disinfecting water sources such as cooling towers. Erythromycin remains a commonly used treatment for infections caused by L. pneumophila.
Brucella Infections in Humans
Brucella species primarily infect domestic animals. However, several species, B. melitensis, B. abortus, and B. suis, can also cause brucellosis in humans. Infection usually occurs through direct contact with infected animals, inhalation of contaminated aerosols, or consumption of unpasteurized dairy products. Today, occupational exposure, particularly among veterinarians, butchers, and slaughterhouse workers, most often causes the disease.
Human brucellosis typically presents with fever, chills, night sweats, headaches, and persistent muscle and joint pain, often progressing into a chronic condition. After entering the body, the bacteria multiply in lymph nodes and spread through the bloodstream. Macrophages in organs such as the liver, spleen, and bone marrow then take them up, where the bacteria survive and multiply within the cells. Because the bacteria live inside host cells, antibody responses alone are not sufficient to eliminate the infection; effective defense relies mainly on cell-mediated immunity, often leading to the formation of granulomas. These are nodules, composed of macrophages and T lymphocytes, which are similar to those found in tuberculosis.
Diagnosis is usually based on detecting increasing levels of anti-Brucella antibodies in the patient’s blood, as isolating the organism can be difficult. Tetracycline is commonly used for treatment.
Bordetella pertussis and Whooping Cough
Bordetella pertussis is the primary human pathogen of the genus and the causative agent of pertussis, commonly known as whooping cough. The bacterium attaches to the ciliated epithelial cells of the respiratory tract. It produces several virulence factors, including endotoxin, pertussis toxin, heat-labile toxin, and an antiphagocytic capsule that helps it colonize and damage the airways.
Whooping cough mainly affects young children and can be especially severe in infants. The illness causes repeated coughing fits followed by a distinctive “whooping” sound during inhalation. Complications such as bronchopneumonia and secondary infections may occur, particularly in vulnerable patients.
Laboratories confirm the diagnosis by isolating the organism from nasopharyngeal samples using specialized culture media. Doctors commonly use erythromycin for treatment, and routine childhood vaccination has greatly reduced the incidence of the disease.
Conclusion
Aerobic gram-negative rods represent an important group of bacterial pathogens responsible for a wide range of human infections. Organisms such as Pseudomonas aeruginosa, Legionella pneumophila, Brucella species, and Bordetella pertussis demonstrate diverse mechanisms of transmission, survival, and disease production. From hospital-acquired infections and respiratory illnesses to zoonotic and childhood diseases, these bacteria continue to pose significant public health challenges. Understanding their pathogenic features, modes of transmission, and methods of prevention is essential for effective diagnosis, treatment, and control of the infections they cause.
You may also like:
- Coliform Bacteria as Indicators of Water Quality
- Passive and active immunization provide protection against diseases
- Archaebacteria and Their Unique Adaptations
- Pathogenic Clostridium Species and Their Role in Human Diseases

I, Swagatika Sahu (author of this website), have done my master’s in Biotechnology. I have around fourteen years of experience in writing and believe that writing is a great way to share knowledge. I hope the articles on the website will help users in enhancing their intellect in Biotechnology.